Common symptoms of allergic rhinitis include sneezing, nasal itching, runny or blocked nose, and itchy, red, and watery eyes. Management typically involves antihistamines, nasal corticosteroid sprays, decongestants, and in severe cases, immunotherapy. Identifying and avoiding triggers is also crucial for effective management.
Adenoid Hypertrophy
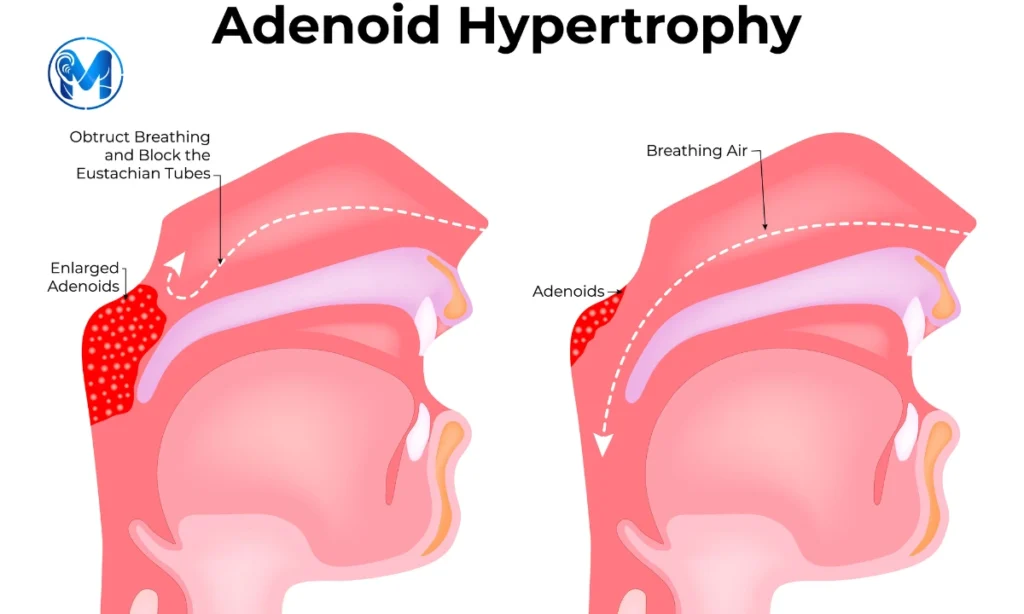
Adenoid hypertrophy constitutes a significant portion of ENT cases that sinusitis treatment doctors in Bangladesh encounter, typically peaking in children aged 2-6 years. This condition is associated with snoring in 7% of cases and sleep apnea in 2%.
Adenoid Hypertrophy description
The adenoids are a pyramid-shaped mass of lymphatic tissue located behind the nose and above the throat. These tissues serve as part of the immune system’s first line of defense, filtering bacteria and viruses entering through the nose. Unlike tonsils, adenoids aren’t visible without special instruments as they sit higher up in the nasopharynx. Normally, adenoids grow during early childhood then gradually shrink by puberty, ultimately disappearing in most adults.
Adenoid Hypertrophy symptoms
Children with enlarged adenoids commonly present with:
- Persistent nasal blockage and congestion
- Mouth breathing, especially during sleep
- Snoring and sleep disturbances
- Hyponasal speech (sounds like talking with a stuffed nose)
- Recurrent ear infections due to Eustachian tube blockage
Furthermore, many children experience drooling of saliva (80%), sleep apnea (30%), and conductive deafness (24%). Severe cases may lead to long-term issues including “adenoid facies” – facial structure changes from prolonged mouth breathing.
Adenoid Hypertrophy causes and risk factors
Adenoid enlargement predominantly occurs from:
- Frequent bacterial or viral infections
- Allergies triggering inflammation
- Environmental factors like pollution
- Passive smoking
Septal deviation ranks as the most common associated risk factor (44.6%), followed by passive smoking (40.8%) and allergic rhinitis (38.5%).
Adenoid Hypertrophy diagnosis methods
Diagnosis typically involves:
- Nasal endoscopy – a flexible tube with camera examines the adenoids directly
- Lateral X-ray of nasopharynx to assess size
- CT scans or MRI for better visualization
- Sleep studies for cases with suspected sleep apnea
Adenoid Hypertrophy treatment options
Initial treatment focuses on addressing underlying causes:
- Antihistamines or nasal corticosteroids for allergy-related cases
- Antibiotics for bacterial infections
Subsequently, if non-surgical treatments fail, adenoidectomy (surgical removal of adenoids) is recommended. This outpatient procedure performed under general anesthesia typically requires only 2-3 days recovery time. Research confirms adenoid removal doesn’t increase infection frequency.
When to see a doctor for Adenoid Hypertrophy
Consult a sinusitis treatment doctor if your child exhibits:
- Persistent mouth breathing or snoring
- Sleep disturbances or pauses in breathing
- Recurrent ear infections
- Speech problems or delayed development
- Symptoms unresponsive to conservative treatments
Obstructive Sleep Apnea (OSA)

Obstructive Sleep Apnea (OSA) ranks among the serious conditions routinely addressed by sinusitis treatment doctors throughout Bangladesh, with studies indicating it affects approximately 24% of middle-aged males and 9% of middle-aged females.
OSA description
Obstructive Sleep Apnea occurs when muscles supporting the soft tissues in your throat temporarily relax during sleep, causing your airway to narrow or close completely. This repetitive collapse blocks normal airflow, resulting in breathing pauses (apneas) lasting 10 seconds or longer. Afterward, your brain briefly wakes you to reopen your airway often so briefly you don’t remember it. This pattern might repeat 5-30 times hourly throughout the night.
OSA symptoms
Nighttime symptoms include:
- Loud snoring
- Witnessed breathing pauses during sleep
- Gasping or choking sensations when waking
- Restless sleep with frequent awakenings
- Nighttime sweating
Daytime effects frequently involve:
- Excessive daytime sleepiness
- Morning headaches
- Difficulty concentrating
- Mood changes and irritability
- Dry mouth or sore throat upon waking
OSA causes and risk factors
Primary risk factors include:
- Obesity – fat deposits around the neck can block airways
- Age – risk increases as you get older
- Male sex – men have 2-3 times higher risk than premenopausal women
- Family history and genetics
- Anatomical factors – large tonsils, thick neck, narrow airway
- Lifestyle habits – smoking, alcohol consumption
- Medical conditions – heart failure, diabetes, hormonal disorders
OSA diagnosis methods
Diagnosis typically involves:
- Polysomnography – overnight sleep study monitoring breathing, heart rate, brain activity
- Home sleep apnea testing – simplified version of sleep study
- Physical examination focusing on upper airway structure
OSA treatment options
Management approaches include:
- CPAP (Continuous Positive Airway Pressure) – most common treatment
- Oral devices/mandibular advancement splints
- Weight loss programs for overweight patients
- Myofunctional therapy – specialized exercises
- Surgery – typically considered when other treatments fail
When to see a doctor for OSA
Seek medical attention if:
- Your partner notices breathing pauses during sleep
- You experience excessive daytime fatigue
- Loud snoring disturbs your or others’ sleep
- You wake gasping or choking
- You have difficulty staying awake during daytime activities
Ear Infections (Otitis Media)
Otitis media accounts for 20%** of Bangladesh sinusitis doctor consultations, ranking as the 3rd most common ENT condition nationwide.
Ear Infections description
Otitis media involves infection or inflammation of the middle ear the air-filled space behind the eardrum containing tiny vibrating bones that transmit sound. This condition occurs in various forms, including acute otitis media (sudden infection), otitis media with effusion (fluid buildup without infection), and chronic suppurative otitis media (long-term infection causing eardrum tears).
Ear Infections symptoms
Common signs include:
- Ear pain or pressure sensation
- Hearing difficulties or muffled hearing
- Fluid drainage from the ear
- Fever (typically low-grade)
Children often display additional symptoms such as excessive crying, ear-tugging, restlessness, balance problems, and reduced appetite.
Ear Infections causes and risk factors
Primary causes include bacterial infections (Streptococcus pneumoniae) and viral infections (respiratory viruses), typically resulting from eustachian tube blockage. Major risk factors encompass young age, bottle feeding instead of breastfeeding, exposure to cigarette smoke, recent respiratory infections, and being male.
Ear Infections diagnosis methods
Diagnosis typically involves physical examination using an otoscope to check for eardrum redness, bulging, or fluid buildup. Additional methods include tympanometry, acoustic reflectometry, and occasionally CT scans for extensive infections.
Ear Infections treatment options
Initial approaches involve pain management through warm compresses and over-the-counter pain relievers. For bacterial infections, antibiotics like amoxicillin are prescribed, though many cases resolve without antibiotics. Severe recurring infections may require ear tube surgery (myringotomy).
When to see a doctor for Ear Infections
Seek medical attention immediately for symptoms persisting beyond 2-3 days, fever exceeding 102.2°F, discharge from the ear, hearing impairment, or symptoms in children younger than 6 months.
Hearing Loss

Hearing loss in Bangladesh affects approximately one-third of the population, making it the second most common form of disability in the country. This sensory deficit creates significant economic, social, educational, and vocational challenges for affected individuals.
Hearing Loss description
Hearing loss refers to complete or partial loss of hearing ability in one or both ears. It can be classified into four types: conductive (affecting outer/middle ear), sensorineural (inner ear damage), mixed (combination of both), and central (nerve pathway issues).
Hearing Loss symptoms
Common signs include:
- Muffling of speech or other sounds
- Difficulty understanding words, especially in noisy environments
- Trouble hearing consonants
- Frequently asking others to speak louder or more clearly
- Withdrawal from conversations
Hearing Loss causes and risk factors
Major causes encompass age-related changes, chronic ear infections (present in 6.2% of Bangladeshis), noise exposure, ototoxic medications, and congenital factors. Certainly, premature birth, oxygen deprivation during birth, and maternal infections like rubella increase risk.
Hearing Loss diagnosis methods
Diagnosis involves physical examination, pure-tone testing, otoacoustic emissions test, and tympanometry. These assessments help determine the type and severity of hearing impairment.
Hearing Loss treatment options
Treatment options include earwax removal, hearing aids, cochlear implants, and corticosteroid medications. Undeniably, early detection and intervention are crucial for effective management.
When to see a doctor for Hearing Loss
Seek medical attention for sudden hearing loss in one or both ears, persistent hearing difficulties, or hearing loss accompanied by dizziness, earache, or pressure sensations.
Vertigo and Balance Disorders

Dizziness and balance problems represent a significant portion of cases seen by sinusitis treatment doctors in Bangladesh, with vertigo affecting 17-30% of the general population. As patients age, these conditions become increasingly common affecting 20% of those over 60, 30% of those over 70, and 50% of individuals older than 80.
Vertigo description
Vertigo is not merely dizziness but specifically the sensation that either you or your surroundings are spinning or moving when no actual movement occurs. This disorienting condition can range from barely noticeable to severely debilitating, sometimes lasting for days and making daily activities extremely difficult. Unlike general dizziness, vertigo is often accompanied by a distinct loss of balance and spatial disorientation.
Vertigo symptoms
Patients typically experience:
- Spinning or tilting sensation
- Dizziness and unsteadiness when walking
- Nausea and sometimes vomiting
- Loss of balance
- Ringing in the ears (tinnitus)
- Blurred vision
- Headaches
Vertigo causes and risk factors
The most frequent causes include:
- Inner ear disorders like BPPV (Benign Paroxysmal Positional Vertigo)
- Vestibular neuritis or labyrinthitis (inflammation from infections)
- Menière’s disease (fluid buildup in inner ear)
- Migrainous vertigo
- Head or neck injuries
Risk factors increase with age, hypertension, diabetes, and previous stroke.
Vertigo diagnosis methods
Physicians utilize several tests:
- Romberg test (standing with feet together and eyes closed)
- Fukuda-Unterberger test (marching in place with eyes closed)
- Video Head Impulse Test (vHIT)
- Videonystagmography (tracking eye movements)
- Vestibular evoked myogenic potentials (VEMP)
Vertigo treatment options
First-line treatments include:
- Medications such as Meclizine and Lorazepam
- Physical therapy with repositioning maneuvers
- Vestibular rehabilitation therapy
- Lifestyle modifications
- Surgery in rare cases
When to see a doctor for Vertigo
Seek medical attention if vertigo:
- Is sudden or severe
- Persists beyond 2-3 days
- Comes with headache, fever above 38°C, double vision, or slurred speech
- Causes persistent vomiting or difficulty walking
- Occurs alongside known stroke risk factors
Throat Infections and Hoarseness

Throat infections and hoarseness rank as Bangladesh’s 5th most common reason for sinusitis doctor visits, demanding precise differential diagnosis for optimal treatment.
Pharyngitis & Laryngitis: Common Throat Complaints
Pharyngitis inflames throat lining, producing scratchy back-of-throat pain. Hoarseness (dysphonia) meanwhile creates raspy, strained, or breathy voice changes.
Hoarseness, or dysphonia, is characterized by a change in voice quality, which may sound raspy, strained, or breathy when speaking or singing. Both conditions can range from mild and temporary to severe and chronic, depending on their underlying causes.
Throat Infections symptoms
Patients typically experience a sore, scratchy throat that worsens when swallowing or talking. Other common symptoms include trouble swallowing, swollen neck glands, red and swollen tonsils (sometimes with white patches or pus), fever, and a hoarse or muffled voice. Hoarseness specifically presents as voice changes, weakness, strain, or complete voice loss in severe cases.
Throat Infections causes and risk factors
Viruses cause approximately 90% of sore throats, including common cold and flu viruses. Conversely, bacterial infections (primarily Streptococcus pyogenes) account for the remainder. Risk factors encompass:
- Occupational voice demands (teaching, public speaking)
- Smoking and alcohol consumption
- Chronic conditions like GERD or allergies
- Age-related vocal cord changes
Throat Infections diagnosis methods
Diagnosis typically involves physical examination, detailed medical history, and visual inspection of the throat. For persistent cases, doctors may perform laryngoscopy to examine the voice box and vocal cords directly. Throat swabs help identify bacterial infections requiring antibiotics.
Throat Infections treatment options
Treatment varies based on cause. Viral infections generally resolve independently within 7-10 days with supportive care. Bacterial infections require appropriate antibiotics. Voice therapy often proves successful for functional and organic vocal disturbances. Chronic laryngitis associated with reflux responds well to anti-reflux medications.
When to see a doctor for Throat Infections
Consult a specialist for sore throats lasting longer than one week, severe throat pain, difficulty breathing or swallowing, fever exceeding 101°F (38.3°C), bloody mucus, recurrent episodes, or hoarseness persisting beyond two weeks.
Comparison Table
| Condition | Primary Symptoms | Main Causes/Risk Factors | Diagnosis Methods | Treatment Options | When to Seek Medical Attention |
| Adenoid Hypertrophy | Nasal blockage, mouth breathing, snoring, recurrent ear infections | Frequent infections, allergies, pollution, passive smoking | Nasal endoscopy, X-ray, CT/MRI scans | Antihistamines, corticosteroids, adenoidectomy | Persistent mouth breathing, sleep disturbances, recurrent ear infections |
| OSA | Loud snoring, breathing pauses, daytime sleepiness, morning headaches | Obesity, age, male sex, family history, anatomical factors | Polysomnography, home sleep testing | CPAP, oral devices, weight loss, surgery | Witnessed breathing pauses, excessive daytime fatigue, loud snoring |
| Ear Infections | Ear pain, hearing difficulties, fluid drainage, fever | Bacterial/viral infections, eustachian tube blockage | Physical exam with otoscope, tympanometry | Pain management, antibiotics, ear tube surgery | Symptoms >2-3 days, fever >102.2°F, hearing impairment |
| Hearing Loss | Muffled speech, difficulty understanding words, trouble with consonants | Age, chronic ear infections, noise exposure, medications | Physical exam, pure-tone testing, tympanometry | Earwax removal, hearing aids, cochlear implants | Sudden hearing loss, persistent difficulties, accompanying dizziness |
| Vertigo | Spinning sensation, dizziness, nausea, loss of balance | Inner ear disorders, infections, Menière’s disease, injuries | Romberg test, vHIT, videonystagmography | Medications, physical therapy, vestibular rehabilitation | Sudden/severe onset, persistence >2-3 days, accompanying symptoms |
| Throat Infections | Sore/scratchy throat, trouble swallowing, hoarseness | Viral (90%) or bacterial infections, smoking, GERD | Physical exam, laryngoscopy, throat swabs | Supportive care, antibiotics, voice therapy | Symptoms >1 week, severe pain, difficulty breathing |
Conclusion
ENT disorders like chronic sinusitis, recurring ear infections, sleep apnea, and hearing loss significantly impact daily life if left untreated. Early diagnosis by a qualified specialist prevents complications and improves quality of life.
Dr. M. Muinul Hafiz, Bangladesh’s leading ENT specialist with MBBS, FCPS, and MS qualifications, offers advanced treatments at his state-of-the-art clinic in Dhaka. From laser surgery to pediatric ENT care, his expertise covers all major conditions.
Don’t delay schedule your consultation today through Contact Us and take the first step toward better ear, nose, and throat health.
FAQs
ENT specialists may recommend antibiotics for bacterial infections, prescription-strength decongestants to open sinuses, and palliative treatments to alleviate symptoms. For chronic cases, they might suggest nasal corticosteroid sprays or even consider surgical options like Functional Endoscopic Sinus Surgery (FESS).
You should consult an ENT specialist if you experience symptoms persisting beyond 12 weeks, recurring sinus infections several times a year, thick green or yellow mucus discharge, or pain when applying gentle pressure around your nose, forehead, or eyes. Additionally, seek medical attention if over-the-counter treatments provide no relief.
The most common ENT problems in Bangladesh include chronic sinusitis, allergic rhinitis, deviated nasal septum, nasal polyps, tonsillitis, adenoid hypertrophy, obstructive sleep apnea, ear infections, hearing loss, vertigo, and throat infections with hoarseness.
Chronic sinusitis is typically diagnosed through physical examination, nasal endoscopy, and imaging tests like CT scans. Treatment options include nasal saline irrigation, corticosteroid sprays, antibiotics for bacterial infections, and in some cases, surgery such as Functional Endoscopic Sinus Surgery (FESS).
Common symptoms of allergic rhinitis include sneezing, nasal itching, runny or blocked nose, and itchy, red, and watery eyes. Management typically involves antihistamines, nasal corticosteroid sprays, decongestants, and in severe cases, immunotherapy. Identifying and avoiding triggers is also crucial for effective management.